Hypertrophic cardiomyopathy
Overview
Hypertrophic cardiomyopathy (HCM) is a cardiac condition where part of the heart muscle is thickened (hypertrophy). This usually takes place in the wall (septum) between the two bottom chambers (ventricles) of the heart. As a result, it blocks or reduces the blood flow from the left ventricle to the aorta and forces the heart to pump harder.
HCM is the most common genetic heart disease in Europe and the USA, with an estimate of 1 person for every 500. It can be passed from parents to children, and when someone has been diagnosed with HCM, first degree relatives, which include siblings and parents, should also be checked.
Symptoms
Many people with hypertrophic cardiomyopathy don’t have any symptoms, while others may only feel symptoms when they exercise. Signs and symptoms of HCM include shortness of breath, exertional chest pain, dizziness, fainting, fatigue, swollen legs, or palpitations, which are the sensation of a fast, fluttering or pounding heartbeat.
Diagnosis
If you have any symptoms of an HCM, or if someone in your immediate family was diagnosed, your medical team may recommend further testing. These include:
An electrocardiogram (ECG) measures the electrical activity of your heart. It can check whether your heart is beating regularly and show the pace of your heartbeat.
Echocardiogram a test that uses ultrasound to create imaging of the beating heart. An echocardiogram can estimate if the heart chambers and valves are healthy or damaged.
Trans-oesophageal echocardiogram gives a more detailed imaging of the heart structures. The doctor will use a small probe that will inserted through the mouth down to a structure called oesophagus (a tube that connects your mouth to the stomach). A light sedation is required for this procedure, to make the patient comfortable.
Cardiac MRI. Magnetic resonance uses powerful magnetic fields to build a detailed image of the cardiovascular system. It’s a non-invasive test and can give multiple figures with regards of the heart condition. It can help to evaluate the anatomy and function of the heart chambers, heart valves, size of and blood flow through major vessels, and the surrounding structures such as the pericardium. It can diagnose a variety of cardiovascular disorders including anomalies like HCM.
A Holter monitor test involves attaching sensors to adhesive pads that are placed on your chest and connected to a portable device that records your heart’s electrical activity during your normal day, usually for 24 or 48 hours. This test checks how your day-to-day activities impact your heartbeat, and whether your heartbeat remains regular over a long period of time. During this test you will also be asked to keep a log of what you did, noting for example when you ate, when you slept and what sorts of tasks you performed.
Genetic testing can show if HCM runs in your family, and is particularly useful if you have a close relative who is diagnosed with HCM, but you don’t exhibit any symptoms. It can also reveal the chances of parents passing the genes on to their children.
Treatment
Medications may be prescribed to help manage and partially relieve your symptoms, however depending on the severity of your case, your medical team may recommend surgical or interventional treatments.
A septal myectomy, also called septal reduction therapy, is a surgery where part of the thickened, overgrown heart wall is removed, and as a result, blood flows more easily. During the operation, the patient undergoes general anesthesia. In some cases, the cardiac surgery team may be able to perform minimally invasive heart surgery, where smaller incisions than those made for open-heart surgery, are used. After a consultation, a cardiac surgeon will arrange all the necessary tests prior to the operation.
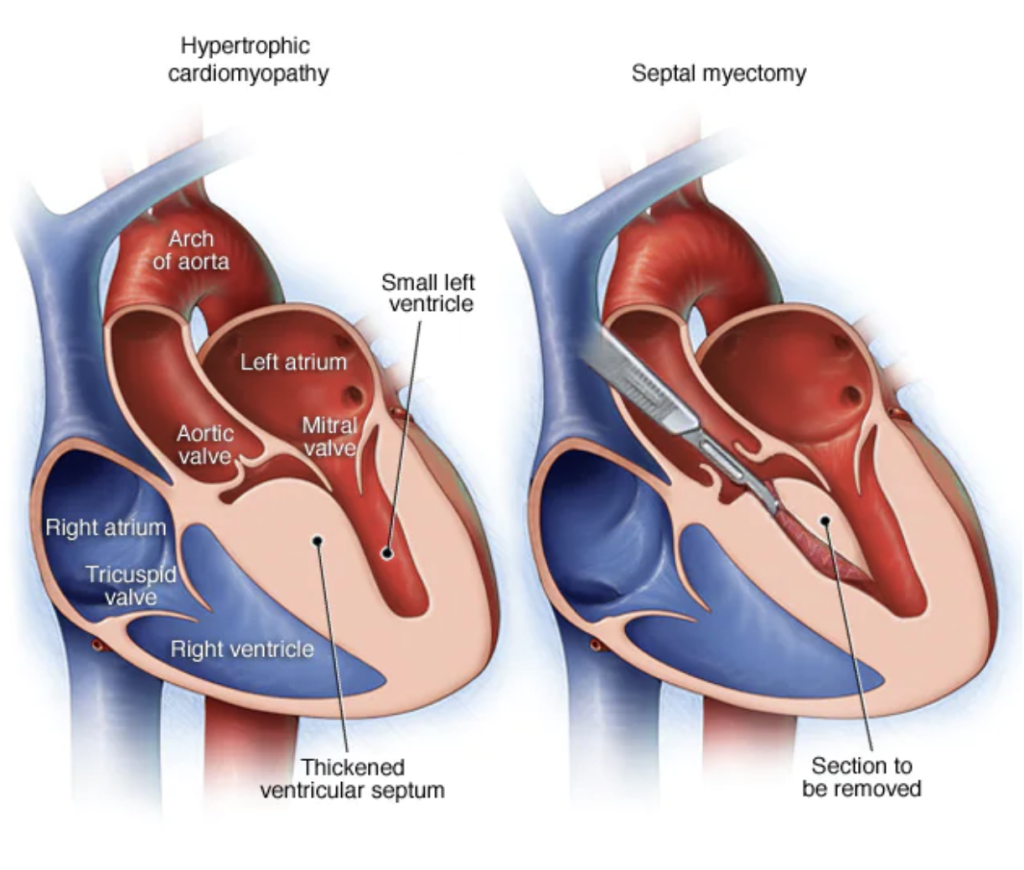
After the operation, the patient will stay in our cardiac intensive care ward for 1-2 days while they recover, then they will be transferred to our regular ward. The average hospital stay after a septal myectomy is 5-7 days, but this varies depending on the patient’s pre-operative clinical condition.
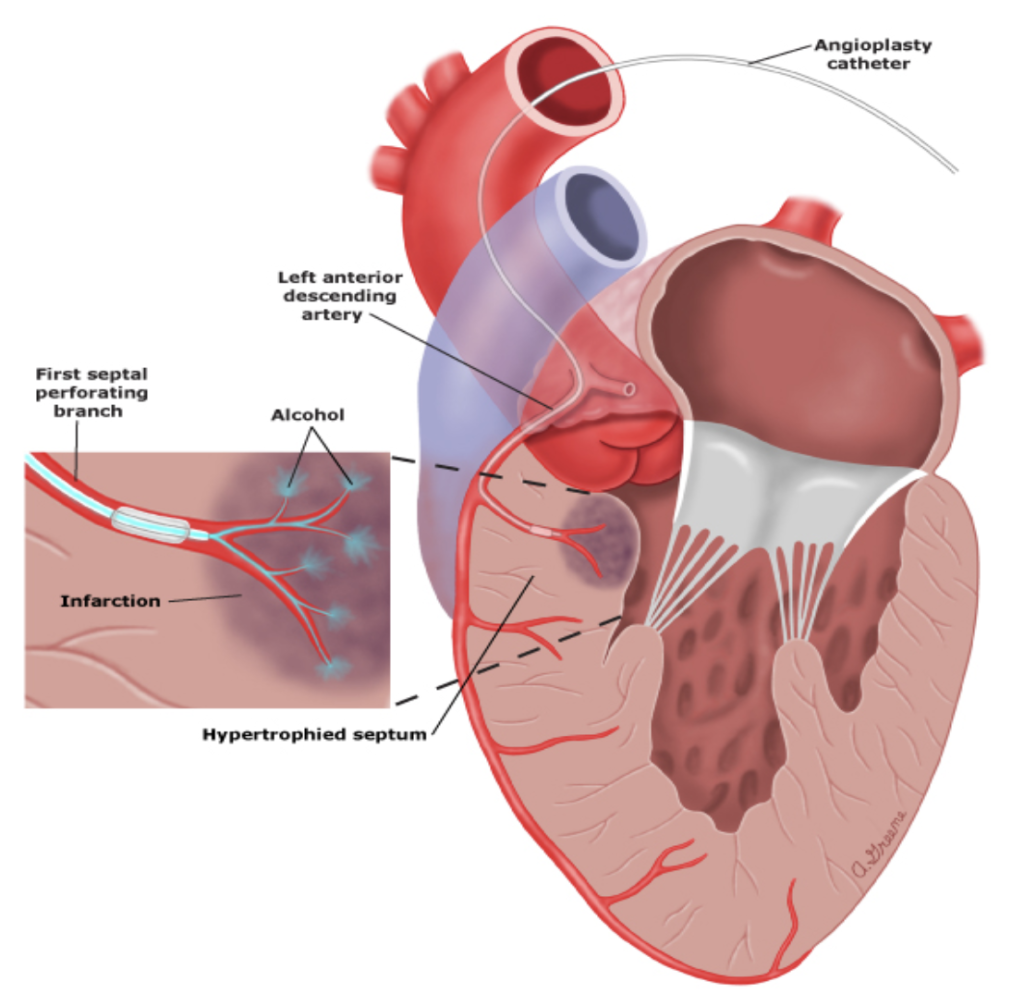
An alcohol septal ablation is a percutaneous procedure where ethanol (a type of alcohol) is injected through a tube into the small artery that supplies blood to the area of the thickened heart muscle This causes the tissue to shrink to a more normal size. It’s recommended for older patients with other medical conditions who are not suitable for surgical operation.
Why GMI
At the GMI, we have a state-of-the-art facility for patients affected by cardiac diseases, which includes our Cardiovascular Diagnostic Center, Cardiology Catheterization Laboratory, Cardiac Surgery Theatre, Hybrid Theatre and Cardiac Intensive Care Unit.
Our team of internationally recognized heart doctors (cardioradiologists, cardiologists, cardiac surgeons and cardioanaesthetist) will guide you through the whole process, from your diagnostic work-up to your treatment and post-treatment care. We are committed to providing the best treatment options to each of our patients. The GMI team will never offer a simple “one size fits all” approach to any patient. We believe each patient’s case is as individual as they are and strive to find the best solution for each of our patients, taking their specific case and diagnosis, their lifestyle, and choices into account.



